Heart Rate Variability (HRV) Measurement Timing: Morning or Night?
a look at stressor timing and measurement position
In this blog, I would like to highlight two key aspects to consider when deciding which measurement protocol or device to use for heart rate variability (HRV) measurement.
In particular, both measurement protocols can provide us with useful data to track long-term changes in physiological stress as it relates to training and health. However, there are important differences.
For example, night measurements happen earlier, and therefore tend to be more tightly coupled with our behavior the previous night. Night data often simply reflects eating and drinking behavior, more than our ability to assimilate additional stress on the following day (despite their use in readiness or recovery scores!).
On the other hand, morning measurements are more tightly coupled to our ability to assimilate additional stress for the day, as they happen after the restorative effect of sleep, and farther away from the previous day’s stressors. Similarly, measurements taken while sitting or standing are often recommended for morning HRV measurement as they capture stressors not visible in night data (such as overtraining, see here), but these measurements are of course unfeasible when measuring in the night. Thus, for daily guidance and training adjustments, morning measurements are more useful than night data collected with wearables.
In this blog, I’d like to discuss in more detail the aspects just mentioned above, and in particular, stressor timing and measurement position, since both these aspects impact the data’s sensitivity to stressors and its interpretation or actionability.
Let’s get to it then.
Stressor timing
We measure HRV because it is a marker of the body’s response to stress. If we want to capture such a response in a meaningful and actionable way, we need to measure it in a reproducible context, at rest, far from other transitory stressors that would confound the measurement. Typically, this means in the morning or the night - and not continuously.
Measuring right after a stressor would be less informative: we would have a suppression in HRV, or increase in HR (e.g. after exercise), and that would be normal. What we are interested in is not this immediate change, but how our system responds to that stressor, which can be better determined by measuring at rest, hours after the stressor (again, in the morning or the night). Failing to bounce back to normal from the stressors after several hours, for example, highlights a negative stress response, or the presence of additional stressors (e.g. lifestyle-related).
If we experience late stressors (evening workouts, a large dinner, alcohol intake, etc.), this might impact our night data to a greater extent. The night comes first, and therefore our HRV is suppressed even if we might have bounced back by the morning. Wearables are convenient and heavily marketed, but night data might in fact miss the point when it comes to morning readiness or recovery, due to measurement timing, especially if you work out in the afternoon or evening or if you periodize your nutrition depending on the upcoming workouts (e.g. having more carbs the night before a hard session), as many endurance athletes do.
Analyzing a response to a workout at different time points (night, and then morning) simply shows how physiology gradually returns to normal, but this has implications for the interpretation and guidance provided.
Example: stressor timing
Below is an example of night data (left) and morning data (right). The morning data is collected while seated, using the phone camera in HRV4Training. The night data is collected using a wearable device.
As described in the image, here we have data collected during a period of periodized nutrition, in which there is higher carbohydrate intake in the evenings (and the mornings) before a hard workout. This is of course beneficial to high-intensity exercise, but the wearable is unable to provide a view of the body’s ability to assimilate additional stress on a given day, as it simply reflects the (already known) change in diet/behavior.
As an athlete or coach, strive to understand how resting physiology and metabolism work (as opposed to falling for marketing claims). It should be clear that there is no point in using a wearable if you want to use the data to capture your body’s ability to assimilate additional stress and to eventually guide training.
The data differs due to stressors and measurement timing, and we need to be aware of these aspects if we want to use the data for guidance or to interpret the body’s response to stress. Wearables mostly tell you what you know already, as the data is tightly coupled to your eating and drinking behavior, and not much else.
Looking at the data above, I can derive that I was ready to execute (and benefit from) a hard session since my morning physiology was within my normal range and glycogen stores were topped up. However, night data (and derived made-up scores such as readiness/recovery) might make you think otherwise (with potential negative psychological implications).
Measurement position
Another big difference between morning and night measurements is that in the morning we can measure in different positions (lying down, sitting, or standing), while during the night, this is unlikely to happen.
Why is measurement position important? When lying down - and especially during sleep, HRV represents parasympathetic activity during undisturbed rest. On the other hand, sitting or standing HRV represents parasympathetic activity in response to a small physiological stressor (that is, changing body position). The physiological challenge exacerbates your response so that if something is off (there is more stress, sickness, or anything else), there will be a much larger change in HRV (and resting heart rate) with respect to the change you would see if you are lying down (sleeping or in the morning). This is why for example, research shows that overtrained athletes had no differences in their night HRV, but a suppression in their morning HRV (sorry, wearables).
Thus, an orthostatic stressor, which here means measuring while sitting or standing, makes it so that HRV becomes more sensitive to the stressors you are facing, and therefore more useful. This is why I recommend measuring while sitting. For more details on these mechanisms, please check out Andrew Flatt’s great blog here.
Measuring while sitting or standing can be particularly beneficial if your heart rate is low, e.g. low 50s or lower, since parasympathetic activity is already high. Measuring while sitting or standing, you might also be less prone to another issue of measurements taken lying down, parasympathetic saturation (a situation in which your HRV measurement does not reflect parasympathetic activity, basically your HRV would be suppressed despite actual parasympathetic activity being elevated). This is particularly true if your training volume is high.
Personally, I measure while sitting, and therefore can only do this first thing in the morning, as opposed to during the night.
Example one: measurement position, sickness
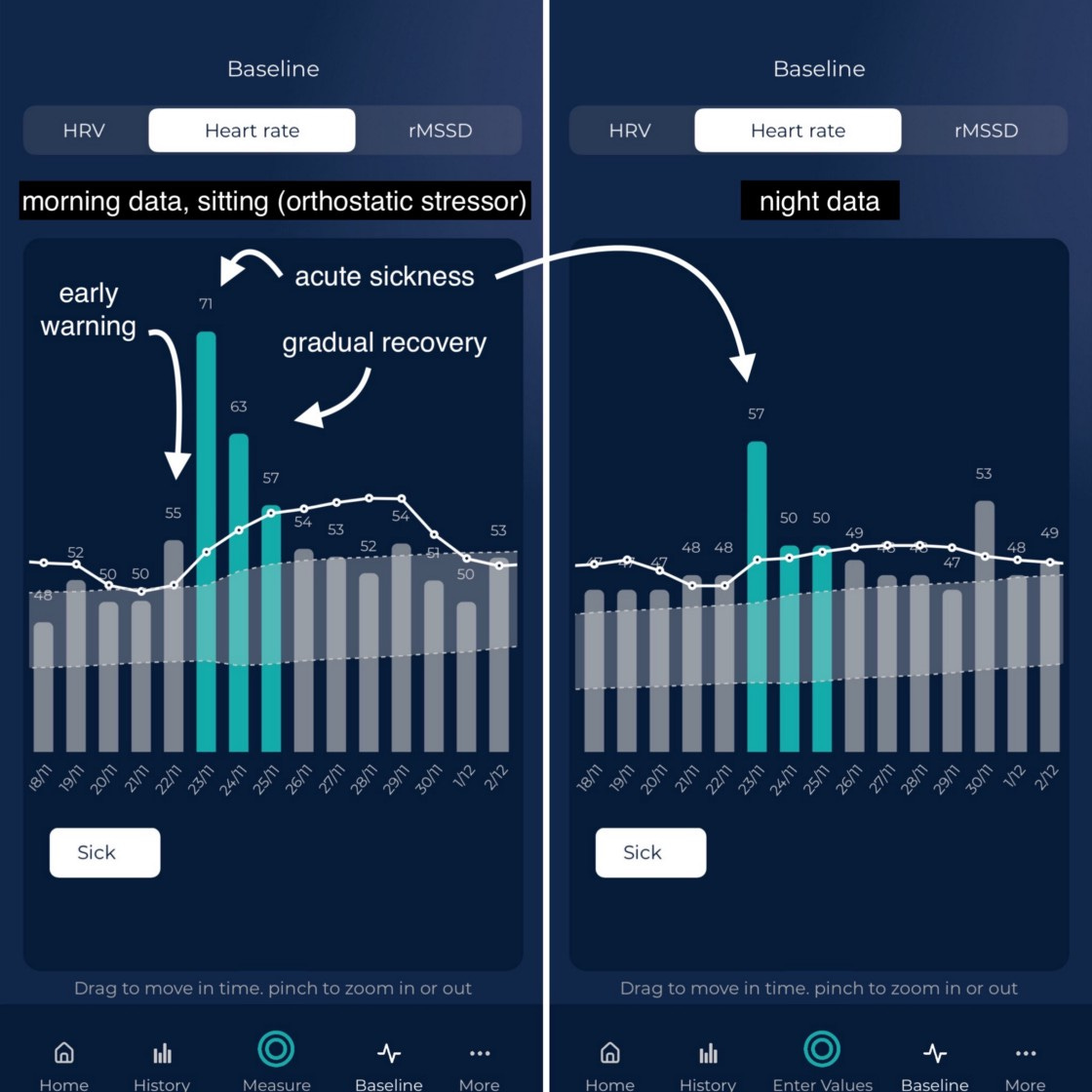
Below is an example showing acute sickness, and how the orthostatic stressor (i.e. sitting in the morning for a measurement) captured very well the acute phase, possibly with an early warning, as well as the recovery phase, while night data failed to capture the recovery phase, and shows a change only during acute sickness (one day).
This is perfectly in line with what we expect: when we have a very large stressor, like the first day of acute sickness, our physiology is altered the entire day or night, and we can easily capture it. As I start feeling better, the following days, measuring in a highly parasympathetic state (while sleeping) provides no useful information, heart rate is only 1 or 2 bpm from where it was before the sickness.
On the other hand, adding a little stressor before a morning measurement (just sitting up), amplifies my response, and I can see very clearly how I am progressing towards renormalization. Despite my heart rate during the night being 50 bpm or 49 bpm every night, as soon as I sit up and measure, I have a marked difference in the response: the second day is 63 bpm, then 57 bpm, and then 54 bpm, clearly capturing my recovery from sickness. This is the orthostatic stressor at work.
Example two: measurement position, travel, and training
Here we move towards more subtle stressors, which are the real reason why HRV can be useful, as for sickness (or excessive alcohol intake, everyone’s favorite sad examples), heart rate would be enough.
Let’s look at travel and training intensity. In the top plot, we can see the morning HRV taken while sitting up. As discussed a few times, this is a protocol that makes it easier to capture your stress response.
We can indeed see that both travel (color-coded) and high-intensity training (I used RPE as a simple marker of intensity) have an impact. Despite baseline HRV being still within the normal range. We have three suppressions below the normal range in the last week when looking at morning data. This added variability due to suppressions and quick rebounds within normal range, is what is captured by the coefficient of variation, another important metric to determine your stress response, which you can find in HRV4Training: a higher coefficient of variation is often associated with a less than ideal response.
In night data, none of this is visible: there are zero suppressions. Sleep is a highly parasympathetic state that is less useful for capturing your stress response, especially in endurance athletes who tend to have quite low resting heart rates. Data collected in the morning, while sitting, challenges the body in a way that makes it possible to capture more relevant responses.
Keep in mind that there's more in the data than just averages and normal ranges, the variability in the data itself, over a few days (i.e. the coefficient of variation), can provide additional insights (something not used in any wearable, but also available in HRV4Training under the HRV trends analysis).
Morning data, in this case, allows us to understand that we are in a situation where we are still able to cope with the stressors imposed on the system (i.e. we bounce back right after a suppression), but that we are probably at our limit (frequent suppressions, increased coefficient of variation). A good moment to make some small adjustments to either reduce stressors or prioritize recovery, quite possibly. None of this is visible in the night data (bottom plot).
What does the research say?
Early research comparing morning and night data is in line with what I have discussed in this blog.
In particular, Christina Mishica and co-authors looked at the correlation between night and morning data and found that “heart rate and RMSSD obtained during nocturnal sleep and in the morning did not differ” (see “Evaluation of nocturnal vs. morning measures of heart rate indices in young athletes”). This is expected when we look at the data at the group level, meaning that if a person has a relatively low HRV, it tends to be low both in the morning and during the night.

However, the analysis above does not look at how data changes in response to stressors, for example how morning and night data respond differently to a workout, something I’ve discussed above. A new article by Olli-Pekka Nuuttila and co-authors tries to address this issue, looking at how HRV collected in the morning and during the night relates to prior stressors. The authors report:
“It could be argued that the morning .. being further away from previous stressors and closer to the following, would provide more relevant information on the current state of homeostasis”
“Furthermore, it can be speculated that nocturnal recordings would rather reflect the physiological and psychological load of the previous day than the actual state of recovery and readiness to perform on the following day”
Stressor timing matters, and in the context of training, morning data might better represent your recovery and ability to assimilate additional stress on a given day.

Finally, when looking at morning vs night data in the context of actual outcomes, such as overtraining, we can see how only morning data is sensitive to these stressors, while night data does not capture any difference (full text here):

To conclude, an overview of recent research (Gronwald et al. 2024) suggests that morning HRV is the more effective option due to the orthostatic test.
If you want to learn more, check out this blog, in which I provide an overview of what the orthostatic test is and add practical tips to exploit this mechanism during your morning measurements without adding unnecessary complexity.
Takeaways
The whole point of using HRV is to capture the body’s response to training or other stressors. Both morning and night data can capture similar long-term trends in our physiology (when measured using validated tools, and following best practices). However, there are some important differences.
Night HRV can be useful to better understand (rather obvious) aspects of your behavior: eating habits, alcohol intake, weight loss, and exercise timing, for example. Similarly to morning measurements, night data can also track quite well anything health-related (acute sickness). However, measuring in the morning, after the restorative effect of sleep is a better time to assess your state and readiness for a new day (and of course, it will also reflect sickness, excessive alcohol intake, etc., as shown in our research). Measuring closer to the previous day’s stressors (i.e. in the night), we might not capture the response effectively (how we recovered after e.g. 10–15 hours, before the next workout).
Additionally, the high parasympathetic state during sleep makes the data less sensitive to stressors. Measuring in the morning, while sitting, adds a little orthostatic stressor that makes the data more representative of our capacity to assimilate additional stress on a given day.
Needless to say, there are practical considerations too, in terms of cost and compliance for example, which might motivate picking one method over the other.
All good as long as we understand what we are doing beyond marketing claims.
I hope this was informative, and thank you for reading!
See also:
Marco holds a PhD cum laude in applied machine learning, a M.Sc. cum laude in computer science engineering, and a M.Sc. cum laude in human movement sciences and high-performance coaching.
He has published more than 50 papers and patents at the intersection between physiology, health, technology, and human performance.
He is co-founder of HRV4Training, advisor at Oura, guest lecturer at VU Amsterdam, and editor for IEEE Pervasive Computing Magazine. He loves running.
Social:







Thank you for the article! Are you aware of any wearables with the option to automatically sample morning data, Marco ?
Firstly thanks for your great content both on here and on your other channels.
My question is around reliability of data (or how much I can trust HRV):
- Each morning I'll wake up, go to the toilet and then return back to my bed where I'll sit on the edge of it and then trigger a 1 minute reflection in the mindfulness app.
- I'm finding that my HRV is a lot higher than I do this (around the 100 mark give or take small fluctuations). If I don't do this protocol the HRV is a lot less.
- Also, if I have alcohol I can sometimes notice that my app tells my HRV is very low but if I then do my morning protocol the scores can shoot right back up (not always thought) around the 120ish mark.
My context: I'm training for a marathon right now and have been doing a lot of zone 2 running for about a year but I'm no athlete. Your journey that you've shared from where you started around be patient with progress is a motivation for me! I use an 80/20 endurance training plan.
Do my results make sense? I suppose I'm questioning these positive responses in terms of reliability.