Heart rate variability (HRV) measurement position: lying down, sitting or standing?
rationale, physiological mechanisms, research and practical recommendations
In the past year, I’ve started recommending measuring HRV while sitting, as opposed to lying down. I came to this conclusion after several conversations with a trusted expert in the field (Andrew Flatt), self-experimentation in different positions over an entire year (so that I could look at the relationship between the data and various acute and chronic stressors), and reading the available literature.
I now consider sitting the best and most effective way to capture data.
In this post, I would like to elaborate more on why this is the case, covering the rationale, physiological mechanisms, and research and providing some practical recommendations.
Rationale
To assess the health of a system, it might be more useful to look at how it responds to a challenge. For example, heart rate and blood pressure changes in response to certain tasks (e.g. coughing, respiration, the Valsalva maneuver, and postural change) have been used to assess autonomic nervous system function in health and disease.
Hence, simply changing posture, provides a challenge to the body, which needs to re-adjust in a number of ways (see next section), and therefore makes our HRV measurement potentially more sensitive to stressors, and therefore more useful.
When we measure while lying down, we are in a highly parasympathetic state, and as such, this state might not be as sensitive to stressors (later we’ll also look at some data to back this statement).
In short, as Andrew put it, “how you adapt/adjust to postural change may better indicate how you adapt/adjust to training” (private communication).
Physiological mechanisms
When we change body position, we have hemodynamic and autonomic re-adjustments as the body counteracts gravitation pull and the displacement of blood towards the lower body.
In particular, we have an increase in sympathetic activity and a reduction in parasympathetic activity (vagal withdrawal). Blood pressure remains fairly constant, while cardiac output decreases and heart rate, as well as total peripheral resistance increase. The change in peripheral resistance is due to increased sympathetic activity (as assessed by measuring pulse-synchronous bursts in peroneal muscle nerve fascicles or by autonomic blockade) and to the baroreflex.
Together with this increase in sympathetic activity, we also have vagal withdrawal, (or reduced parasympathetic activity) which has been clearly documented by pharmacological studies. Vagal withdrawal is likely driving the change in heart rate.
Below we can see how atropine injection (inhibiting the parasympathetic system) shows no rebound in heart rate when changing position. If the parasympathetic system is inhibited, the heart rate stays elevated (RR interval duration reduced), and there is no rebound to the values we had before changing body position.
Hence, when you change body position, it is the parasympathetic system that quickly re-normalizes heart rate. This means that by measuring shortly after changing body position, you capture the activity of the parasympathetic system and how it responds to the challenge of changing body position. That's exactly what you want to measure with HRV (because HRV cannot capture anything else).
This is also reflected in clinical practice, where a lack of response to an orthostatic stressor (e.g. heart rate or HRV not responding as expected when changing body position, for example remaining constant), are markers of pathological conditions.
Research
So far I’ve discussed the rationale and shown the physiological mechanisms that make sitting or standing measurements potentially superior to measurements taken while lying down, in the context of assessing the body’s readiness for the day via HRV analysis.
This hopefully all makes sense, but as usual, we need to look at some data to determine if in practical terms, this is indeed the case, or if maybe, these differences are not of practical utility. Below I report the findings of a few studies that looked at longitudinal data collected in different body positions (there aren’t that many!) in relation to different stressors or performance. I will also add some of my own anecdotal data, which also shows some of the issues with a lack of sensitivity to stressors when measuring while lying down.
Fitness
Starting with using HRV as a predictor of VO2max (not really something we should be doing), we have that only 2 out of 30 HRV parameters correlated significantly with VO2max when the measurements were taken while supine, while 15 out of 30 parameters correlated significantly when measuring while standing. Hence, measuring while sitting seems at least more sensitive to changes in fitness.
Psychological stress
Another interesting study looked at mental stress. I think this is a good one because I believe these are the stressors we need to consider when using tools like HRV (on my end, it’s kind of sad to see that the proliferation of HRV tools mostly leads to people sharing changes in their wearables data only when they get wasted, something you certainly do not need HRV for - pardon my digression). Back to the study, in this case, the authors found that a higher incidence of stress symptoms was associated with lower HRV during the orthostatic test after awakening. This association was found during both supine rest and standing, but not during night HRV, collected while sleeping. In this case, being awake was enough of a stressor, and both body positions provided the same insights (and both were superior to night data).
In a recent study, orthostatic measurements were taken and analyzed in relation to mental health (depression index). As the authors reported, only a weak linear relationship was found between rMSSD during rest upon waking and rMSSD while standing upon waking, highlighting how these two measurements are not necessarily the same. Most importantly, although measurements taken while lying down at rest showed only a weak linear relationship with psychological indices, measurements taken while standing showed moderate relationships.
Training: overtraining and altitude
Moving to the response to training, attenuated HRV responses were found when measuring in the upright posture, after supine rest, in overtrained athletes. Similar findings were reported also by another study, looking at cognitive tests in overtrained athletes.
In yet another study, overtrained athletes were again compared to controls. HRV did not change between overtrained athletes and controls during sleep, but there was a reduction in HRV for the overtrained group when measured after awakening. The authors explain how awakening itself enhances the sympathetic tone, and how burnout patients have shown elevated cortisol levels during the first hour after awakening, a sort of overreaction that could also be present in overtrained athletes (as highlighted by a reduced HRV only after awakening). Below we can see the difference in HRV between the two groups.
Finally, in this study, we can see how an even simpler measure influenced by autonomic activity (heart rate), changes more when sitting with respect to lying down, in response to altitude. The difference between the black and white dot (body positions) is much larger at the beginning of the altitude period, with respect to sea level or the end of the period, after acclimatization. This difference highlights an increased sensitivity to the stressor for sitting data.
Example with HRV4Training
Finally, below is some of my data, where I have seen similar differences to what is shown in the scientific literature I have covered above.
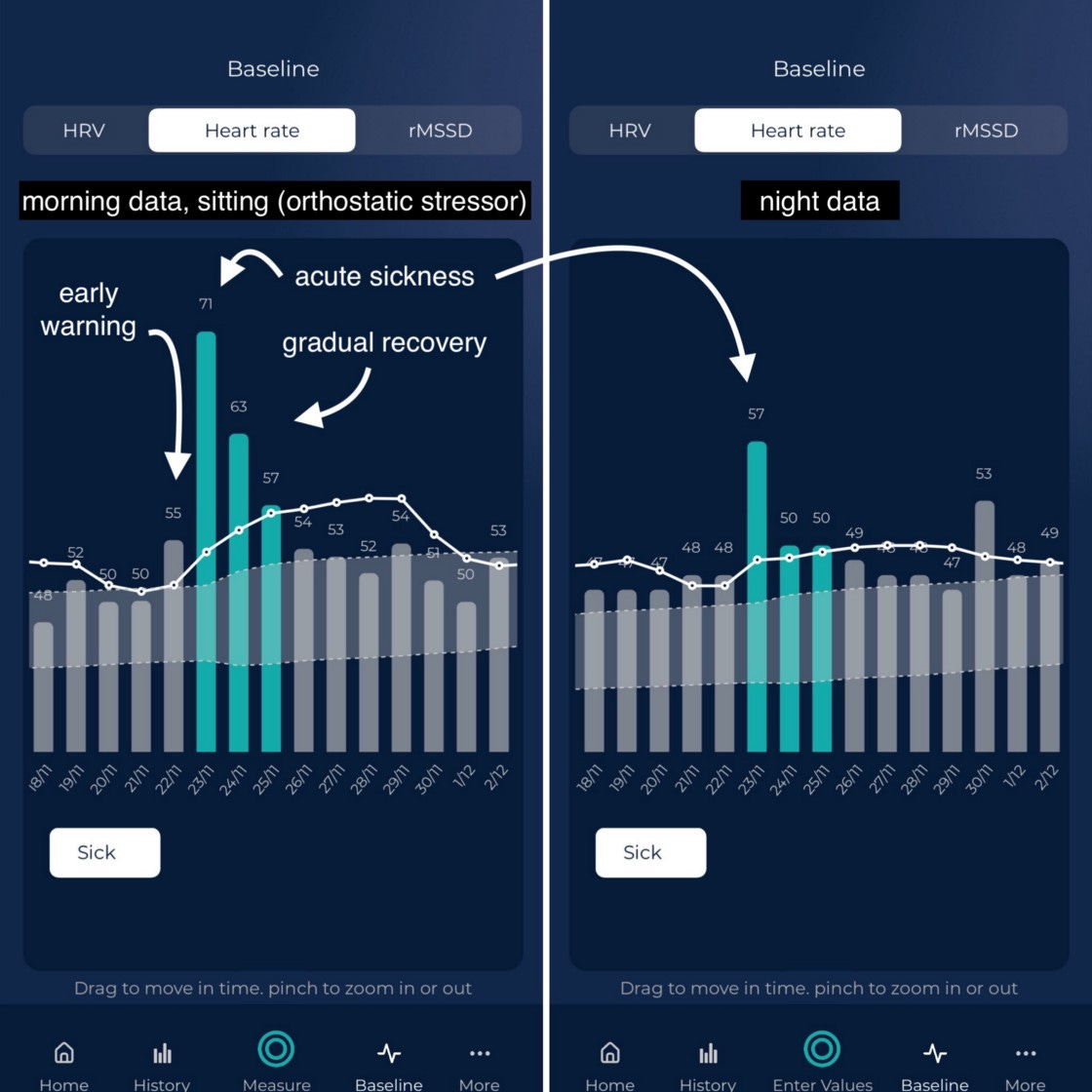
In particular, the data shows acute sickness, and how the orthostatic stressor (i.e. sitting in the morning for a measurement) captured very well the acute phase, possibly with an early warning, as well as the recovery phase, while night data failed to capture the recovery phase, and shows a change only during acute sickness (one day).
This is perfectly in line with what we expect: when we have a very large stressor, like the first day of acute sickness, our physiology is altered the entire day or night, and we can easily capture it. As I start feeling better, the following days, measuring in a highly parasympathetic state (while sleeping) provides no useful information, heart rate is only 1 or 2 bpm from where it was before the sickness.
On the other hand, adding a little stressor before a morning measurement (just sitting up), amplifies my response, and I can see very clearly how I am progressing towards renormalization. Despite my heart rate during the night being 50 bpm or 49 bpm every night, as soon as I sit up and measure, I have a marked difference in the response: the second day is 63 bpm, then 57 bpm, and then 54 bpm, clearly capturing my recovery from sickness. This is the orthostatic stressor at work.
Takeaways and recommendations
When lying down, HRV represents cardiac autonomic nervous system activity during undisturbed rest. On the other hand, sitting or standing HRV represents cardiac autonomic nervous system activity in response to physiological stress.
The physiological challenge exacerbates your response so that if something is off (there is more stress, sickness, or anything else), there will be a much larger change in HRV (and resting heart rate) with respect to the change you would see if you are lying down (in particular during sleep).
Thus, an orthostatic stressor, which here means measuring while sitting or standing, makes it so that HRV becomes more sensitive to the stressors you are facing, and therefore more useful. This is why I now recommend measuring while sitting.
Measuring while sitting or standing can be particularly beneficial if your heart rate is low, e.g. low 50s or lower, since parasympathetic activity is already high. Measuring while sitting or standing, you might also be less prone to another issue of measurements taken lying down, parasympathetic saturation (a situation in which your HRV measurement does not reflect parasympathetic activity, basically your HRV would be suppressed despite actual parasympathetic activity being elevated). This is more likely to happen if your training volume is high.
Personally, I now measure while sitting, and therefore can only do this first thing in the morning, as opposed to during the night. Why sitting and not standing? My main motivation for recommending sitting as opposed to standing is mostly practical: typically it is easier to mess up a measurement when standing, as people tend to be impatient or to move more. Additionally, standing might be “too much” of a stressor (there is a larger increase between sitting and standing than there is between lying down and sitting, in terms of parasympathetic activity). Thus, sitting seems the perfect trade-off to me.
Studies looking at the stability and reliability of rMSSD in different body positions showed no differences (i.e. the data is reliable even when not lying down). However remember that body position needs to be consistent for the data to be interpreted correctly, so use the same body position every day. If you decide to change, give it a few weeks so that HRV4Training can learn your new normal physiological state, and correctly interpret deviations from your normal.
I hope this was informative, and thank you for reading!
Marco holds a PhD cum laude in applied machine learning, a M.Sc. cum laude in computer science engineering, and a M.Sc. cum laude in human movement sciences and high-performance coaching.
He has published more than 50 papers and patents at the intersection between physiology, health, technology, and human performance.
He is co-founder of HRV4Training, advisor at Oura, guest lecturer at VU Amsterdam, and editor for IEEE Pervasive Computing Magazine. He loves running.
Social:







Thank you very much for this piece. Not sure if this matters, but in terms of the timing of measurement after moving - would you recommend that HRV be measured immediately after moving positions from lying to sitting? Or leave a little delay, for example, wait in a sitting position for a few minutes and then measure HRV?
Is it normal for there to be large differences between lying and standing, even when hrv4training says that my trend is stable and to proceed as planned? My lying average rmsdd is around 120 but my standing average is around 25? Also when hrv4training shows my average rmsdd in population comparison or monthly summary, is that lying, standing, or both?
The app is super helpful, just trying to understand a little deeper, thanks Marco!